How can point-of-care ultrasound aid diagnosis and enhance patient care?
This is a question that healthcare providers around the world and working in a whole host of different clinical disciplines are asking. You may have asked the same question. Perhaps you’re considering implementing point-of-care ultrasound (POCUS) at your facility. Or maybe you already use it and have your own experiences to add to the conversation. Whatever your own situation, POCUS is certainly a top trending topic in the world of ultrasound. And it’s one that Dr. David Tierney M.D, Program Director of the IMBUS program at Abbott Northwestern Hospital in Minneapolis, MN, feels strongly about. Dr. Tierney leverages Philips Lumify ultrasound to scan patients conveniently at the bedside, delivering care on the go.
Case study: Patient with an aortic valve vegetation
In one of his cases, Dr. Tierney treated a 22-year-old female patient with a history of asthma. She presented to the emergency department with fever, severe SOB and significant confusion and lethargy and was unable to provide any background. The initial concerns of the triage team assigned to her centered around a recurrent severe asthma exacerbation with an underlying bacterial infection or influenza and severe sepsis. A physical exam, ECG and CXR were performed. The ECG was normal apart from sinus tachycardia and the CXR showed a subtle patchy bilateral interstitial infiltrate. The patient was admitted to the ICU.
Using POCUS in the ICU
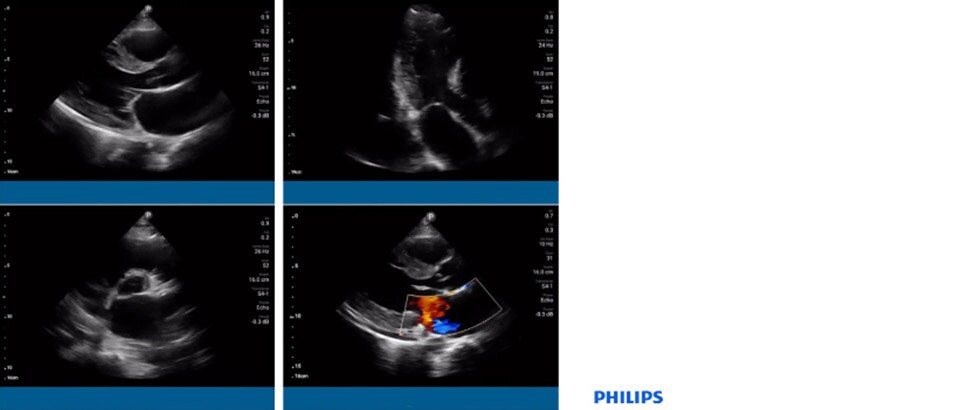
Dr. Tierney used Lumify to performed point-of-care pulmonary and cardiac ultrasound. The lung examination demonstrated findings consistent with bilateral pulmonary edema and pleural effusions without pneumothorax. The cardiac scan showed a mobile aortic valve vegetation and significant mitral regurgitation. In the ICU, the patient developed chest pain with rapidly worsening hypoxia and respiratory failure. She was urgently intubated. Additional POCUS showed antero-septal and apical wall motion abnormalities in the apical 4-chamber view. Her ST elevation MI was considered to be related to a likely embolic vegetation to the left anterior descending coronary artery. In an effort to stabilise her condition, the patient underwent an emergency LAD thrombectomy in the cath lab with placement of a balloon pump and Swan-Ganz catheter. After removal of these devices, POCUS incidentally visualised a mobile thrombus vs. additional vegetation in the IVC.
How POCUS helped
So what was the benefit of portable ultrasound at the point-of-care and how did this impact the medical team’s decision and the patient’s outlook? Having immediate access to ultrasound in the ICU helped Dr. Tierney and his colleagues quickly narrow a differential diagnosis. What’s more, in this case, the exam picked up things not originally included in the differential such as pulmonary edema, mitral regurgitation, and endocarditis. As this example underlines, using POCUS in emergency situations can accelerate triage and improve the time it takes to initiate the appropriate treatment. For more information on this case, watch the presentation. Find more stories at @PhilipsPOCUS on Twitter.