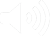More than just a nuisance
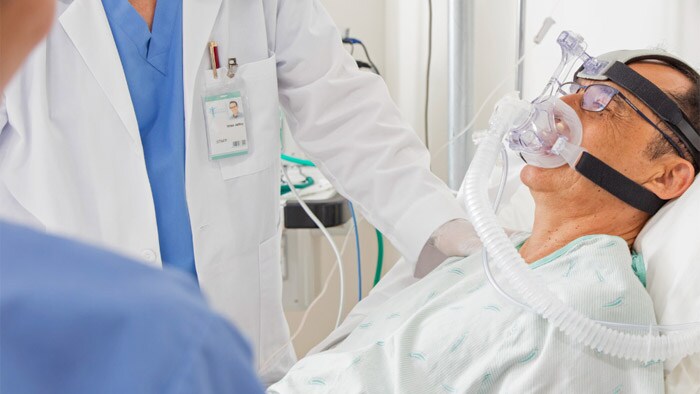
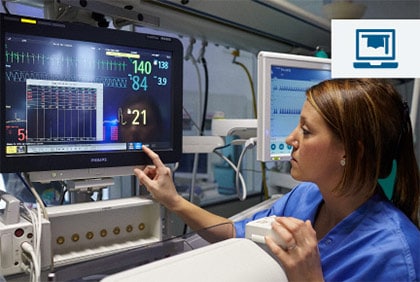
The proliferation of alarms generated by monitoring systems is a growing concern for anyone committed to patient safety. Exposure to excess alarms in care settings, especially non-actionable alarms, can result in desensitisation among the clinicians that they are intended to alert, a syndrome called alarm fatigue.
Alarm fatigue can lead to reflexive silencing of alarms, breaking monitoring protocols and missing true positive alarms—placing a burden on caregivers and jeopardising their ability to care for patients.
When an alarm goes off you want to make sure it is clinically relevant.”
Ineke van de Pol
ICU nurse practitioner, St. Antonius Hospital, The Netherlands
Excessive false alerts
impact a hospital on many levels

Clinical
Missing actionable alarms jeopardises patient safety.

Financial
Patient harm as a result of over-alarming can have costly repercussions from transfers to the ICU, extended length of stay and litigation.

Technical
The lack of alarm customisation for individual patients can create excessive nuisance alarms.

Operational
About 10% of nursing time is lost responding to non-actionable alarms.

Growth A stressful, noise-filled work environment can contribute to staff burnout.

Regulatory
Non-compliance can be costly, as health care moves from volume to value-based care models.
Alarm management 101
Alarms are a good thing… aren’t they? Raise your team’s awareness about alarm fatigue with this module from a Philips alarm management consultant.
This video drills down into the root causes and impact of the problem and shares research on how it is currently perceived.
Alarm management:
become the expert
Philips is
here to help

The price for patients Find out why you should protect your patients
What drives alarm fatigue? Discover new facts and approaches for making effective change

Get some practical guidance Success stories, exclusive case studies and proven solutions
Footnotes: [1] Juniper Consulting. Junicon Web Survey, 2012. [2] Cvach, M., "Monitor Alarm Fatigue: An Integrative Review", Biomedical Instrumentation & Technology, July/August 2012, pp. 268-277.